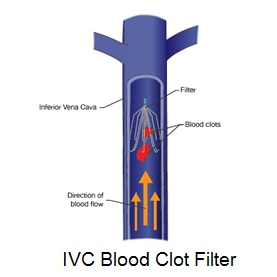
 Bariatric patients (Lap band surgery) implanted with an IVC filter had a higher death rate than those who received no filter during their surgery.
Bariatric patients (Lap band surgery) implanted with an IVC filter had a higher death rate than those who received no filter during their surgery.Bariatric surgical procedures (according to the American Society for Metabolic and Bariatric Surgery) are designed to trigger weight loss by restricting the amount of food the stomach can hold, causing malabsorption of nutrients, or by a combination of both gastric restriction and malabsorption.
“In bariatric surgery, the risks of IVC filter insertion exceed the benefits and their use should be discouraged,” said Jonathan D. Finks, M.D., of the University of Michigan in Ann Arbor.
The most popular bariatric surgery procedures are gastric bypass; sleeve gastrectomy; adjustable gastric band; biliopancreatic diversion with duodenal switch. According to a study published as an abstract in 2011 and presented at a conference, anyone who underwent any of these procedures and was simultaneously implanted with an IVC filter had a higher death rate than bariatric surgery recipients not implanted with IVC filters.
IVC Filter Recipients’ Higher Death Rate
VTE, according to a story in Medpage Today, occurred in 1.8% of 1,045 filtered patients versus 0.4% of a propensity-matched cohort. The 30-day mortality was 0.07% with a filter and 0.02% in a matched cohort of unfiltered patients. Dr. Finks reported the findings in an American Society for Metabolic and Bariatric Surgery meeting.
Analysis of 29,000 unmatched registry patients without filters showed similar disparities in VTE, mortality, and other adverse outcomes in IVC filter recipients compared with unfiltered people.
FDA IVC Filter Safety Alert
Concern about potential risks associated with IVC filters led FDA to issue a safety alert in 2010. The agency said that since 2005 it had received nearly 1,000 adverse event reports related to IVC filters, most involving device migration (328); embolization (146); perforation (70); IVC filter fracture (56).
The FDA recommended medical professionals consider removing retrievable IVC filters and encouraged close follow-up of all filtered patients.
Dr. Finks said investigators in the Michigan Bariatric Surgery Collaborative took notice of IVC-related complications a year or two before the FDA alert. About 8% of Michigan hospitals reported routine use of IVC filters during bariatric surgery. More recent data shows IVC filter use lowered to less than 1%.
No Benefit for PE Risk and Greater Risk of Complications
Previous analysis of the collaborative’s data showed IVC filters did not reduce the risk of pulmonary embolism and trended toward an increased risk of complications (Ann Surg 2010; 252: 313-318).
In further efforts to assess the risk-benefit analysis of IVC filters for bariatric surgery patients, Dr. Finks and colleagues examined the collaborative database for patients who had undergone bariatric procedures from 2006-2011. They found that 1,045 of 31,499 patients received prophylactic IVC filters.
From the patients who did not receive filters, investigators produced a propensity-matched cohort of 1,045 patients for comparison with the filter group.
IVC Filter Risks outweigh Benefits in Bariatric Surgery
Dr. Finks reported that 39% of patients in the filter group had a history of VTE, as did 36% of the matched cohort, both substantially higher than in the 29,409 unmatched patients who did not receive filters.
Dr. Finks disclosed a relationship with Ethicon EndoSurgery.
Related
- IVC Filter Lawswuit
- Bard Filter Lawsuit
- Filter risks trump benefits in bariatrics
by Matthews & Associates




